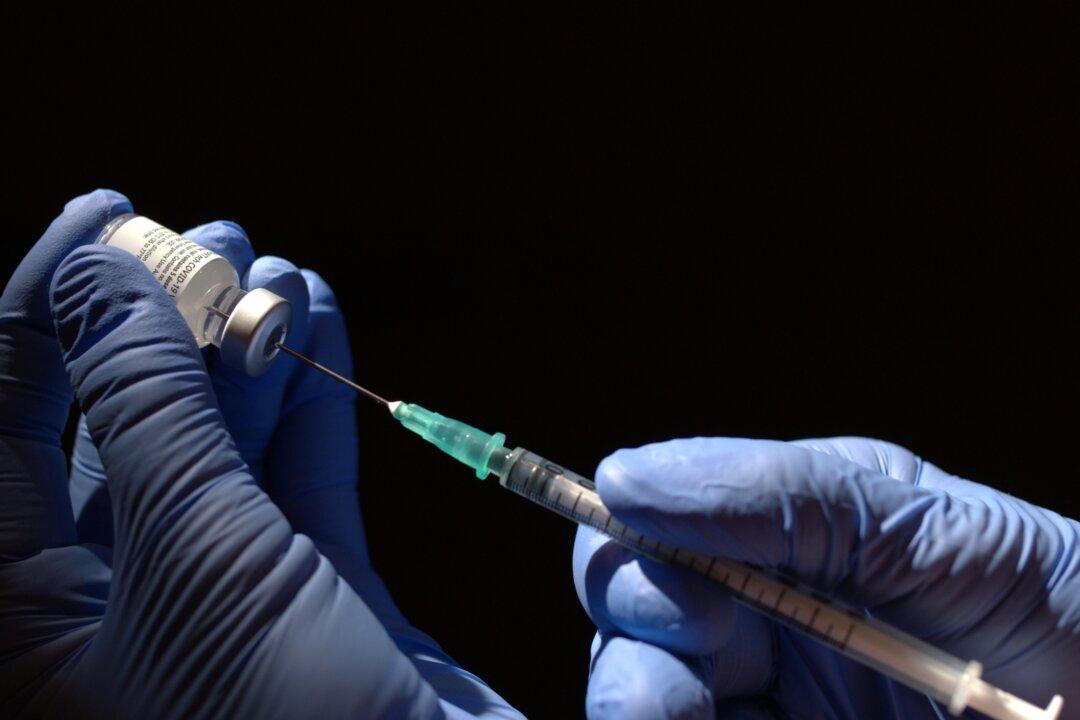
President Joe Biden recently announced his “wartime” strategy to confront COVID-19. His weapon: vaccines. The battle plan builds on former President Donald Trump’s arsenal of 400 million vaccines, with a purchase of an additional 200 million more shots so all Americans can get both their recommended doses faster.
To date, more than 60 million vaccine doses have been distributed in the United States and more than 10 million people have received their first of two doses.